 
Notably, trauma can also lead to exophthalmos in cases of significant orbital swelling or hemorrhage. This often leads to a relative enophthalmos of the affected eye. When an orbital fracture is present, orbital tissue may herniate into the adjacent maxillary or ethmoid sinuses. The position of the globe within the orbit is a valuable measure to obtain. Of note, patients may not complain of diplopia if they have significant eyelid edema obstructing the visual axis, so gently holding eyelids open during motility testing can be helpful. It is useful to gather quantitative measurements with prism bars to better describe and monitor ocular motility. 3-6Ĭomprehensive evaluation of extraocular motilities can be completed in office with an alternate cover test in primary, lateral, and vertical gazes. 2-5 Diplopia may be the result of direct muscle or periorbital tissue incarceration, traumatic hemorrhage and swelling of the orbital tissue, or direct damage to muscles, nerves, or vasculature. In cases of post-traumatic V2 hypoesthesia, imaging is warranted.ĭouble vision is a common symptom of orbital trauma and has been reported in 16 to 56 percent of cases of orbital fractures. In those cases, consider inquiring about new onset numbness or loss of sensation in the upper teeth or lip. 
1 Unfortunately, the use of this technique may be limited in cases of bilateral or antecedent sensation loss. This can be evaluated by testing sensation on both sides of the face in the V2 dermatome and asking the patient to rate sensation (0 to 10) on each side. It passes through the infraorbital canal along the orbital floor and may be damaged in blow-out fractures, leading to hypoesthesia. This nerve branch serves to provide tactile, temperature, and pain information from the midface (lower eyelid to upper lip), nasal cavity, teeth of the upper jaw, and palate. The infraorbital nerve arises from the maxillary division of the trigeminal nerve (cranial nerve V2). While edema and bruising may be fairly common in ocular trauma, they are far from pathognomonic for orbital fractures.īelow are findings more commonly seen in orbital fractures. Patients who present with orbital fractures may complain of a multitude of symptoms including eyelid swelling, ecchymosis, pain, or double vision. Once the globe is evaluated in full, attention is directed to the orbital exam. Timely management of these ophthalmic findings is important for preservation of vision. Trauma severe enough to fracture an orbital wall may present with findings such as iritis, iridodialysis, hyphema, vitreous hemorrhage, commotio retinae, retinal breaks, or in some cases, a ruptured globe. When a patient presents with a history of periorbital trauma, the globe must first be thoroughly evaluated for evidence of injury. Finally, the lateral wall of the orbit is comprised of the zygomatic bone and greater wing of the sphenoid. The orbital roof divides the orbit from the anterior cranial fossa and is composed of the frontal bone and the lesser wing of the sphenoid. It is through this tract that infections may spread from the sinus into the orbit. The medial wall possesses small anterior and posterior ethmoidal foramina that pierce through the wall and communicate with the adjacent ethmoid sinus. The lamina papyracea, translated from Latin as “thin wall,” is part of the ethmoid bone and is the thinnest bone of the orbit. The medial wall is formed by the maxillary bone, ethmoid bone, lacrimal bone, and lesser wing of the sphenoid. The largest paranasal sinus, the maxillary sinus, lies directly below the orbital floor. The infraorbital canal passes within the floor, and the bone medial to it is thin and susceptible to fracturing. The floor of the orbit is formed by the maxillary bone, palatine bone, and orbital process of the zygomatic bone. 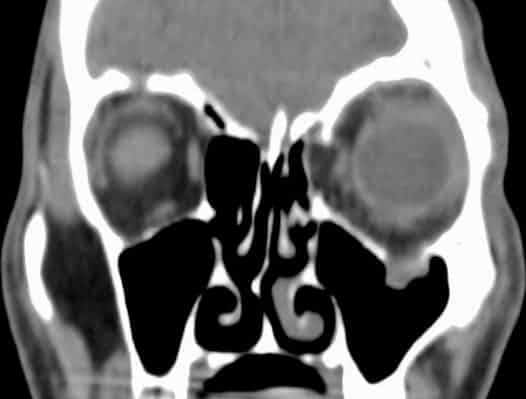
This article will familiarize readers with orbital fractures by reviewing clinical examination techniques, demonstrating common imaging findings, and providing guidance on imaging and referral patterns.įour walls form the boundaries of the orbit. While ophthalmologists are often consulted to evaluate trauma patients, optometrists are less likely to have experience with these cases. Orbital fractures are a common result following trauma, often due to motor vehicle accidents, sports-related injuries, falls, or assault. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
